Blogs and Case Studies
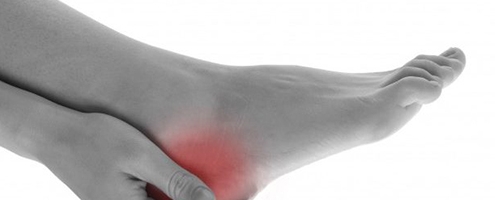
Why do Feet Hurt During Pregnancy?
0 Comments
/
Definition
Pregnancy triggers many different changes in a woman's…

Childrens heel pain and sever’s disease
Pain and discomfort in the younger population is often times associated with body changes and development. A lot of this pain is often dismissed by parents and guardians as ‘growing pains’ that passes as the child develops. Heel pain is particularly common in active kids.

Metatarsalgia – Pain in the ball of the foot
Metatarsalgia is a broad term to generally describe inflammation and pain of the metatarsal bones in the foot. This is a common problem occurring with overuse injuries often seen in people who participate in high impact sports or people who spend extended period of time performing weight bearing tasks with unsuitable footwear.

Different lacing techniques
Did you know that there are a number of different shoe lace techniques appropriate for each foot type. Here at The Podiatry Centre, we are aware that feet are as unique as the patients we see. So above is a lacing chart from our good friends at the Athletes Foot showing a number of ways in…
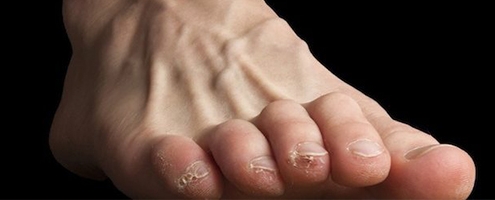
What is a corn and callous, and can you stop them
What are calluses and corns? Calluses and corns are areas of thick skin caused by pressure or friction. It is a normal reaction by the body to produce thick skin when pressure is applied, in order to prevent itself from breaking down.
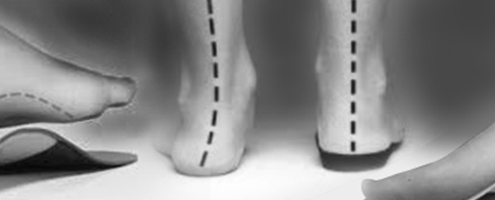
Shoes that fit orthotics
Part of my job when dispensing orthotics to patients, is to educate them on the type of shoes that fit orthotics as is can be often confusing as to what to buy and what to avoid. Fitting orthotics in sport shoes, or lace-up shoes is often a straight forward process with no difficulty.
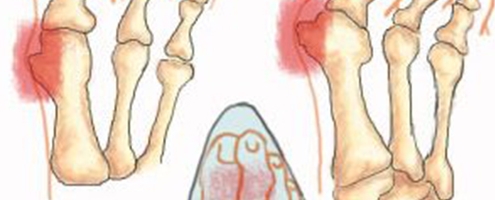
How to treat bunions ?
What are bunions? Medically referred to as “hallux abducto valgus”, bunions are a relatively common deformity found in the fore foot area which is usually characterised by a prominent ‘bump’ and deviation of the big toe from its original position.

Are you wearing the right shoes for Crossfit ?
CrossFit is a fitness phenomenon that has taken the athletic community by storm. It is a regimen of constantly varied, functional movements performed at high intensities within a communal environment.1CrossFit incorporates a variety of exercises into daily workout routines.

Treatment of heel pain plantar fasciitis
What is Plantar Fasciitis? In the running community, plantar fasciitis is the primary cause of pain in the heel and affects as much as 10% of runners. As you run, the Achilles tendon works with plantar fascia (a thick band at the bottom of your feet) to help store energy.
